Scar Management
Have you had a C-section, ACL reconstruction, hip or knee replacement, hernia repair, breast surgery, or another procedure that left an incision?
If yes — don’t skip this.
There are three areas to focus on with scar management
1. Scar Desensitization
2. Scar Massage
3. Scar Appearance
1. Scar Desensitization
(Start Early — Even Before the Dressing Comes Off)
After surgery, the small nerves around the incision are often irritated or temporarily disrupted. This can cause:
Numbness
Dullness or decreased sensation
Tingling
Burning
Hypersensitivity
Sharp, zappy sensations
These symptoms often improve over the first year, but scar desensitization helps the nerves “re-learn” normal sensation more efficiently.
When to Start
You do NOT need to wait until steri-strips or dressings are removed.
You can begin around the area right away (just don’t remove dressings or rub directly over them).
Do it daily — after a shower, while getting dressed, before bed. Consistency matters more than duration.
Spend 2–3 minutes total per day.
How to Do Scar Desensitization
Step 1: Start With Gentle Textures
Gather:
Cotton ball or Q-tip
Soft washcloth
Back of a spoon (for cool sensation)
Technique:
Begin away from the scar in an area that feels like sensation has changed post surgery.
Lightly touch the skin using:
Small circles
Side-to-side strokes
Gentle brushing motions
Slowly work closer to the incision.
Eventually move directly over the scar (if fully healed).
Pressure Guidelines
Pressure should be light.
It should feel strange or mildly uncomfortable — but not painful.
When you stop touching the area, symptoms should settle quickly.
If pain increases afterward, you pressed too hard.
⚠️ Important: Because sensation may be reduced, test your pressure on another body part first so you don’t accidentally press too hard.
Step 2: Progress the Texture
As the area improves, vary the input and try using these items instead:
Makeup brush
Denim (especially important if you want to go back to wearing jeans)
Paper towel
Terry cloth
Gentle vibration (small massager)
This variation helps the nerves tolerate different sensations again
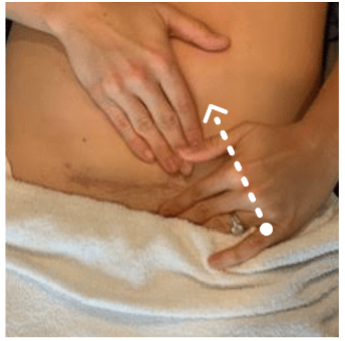
2. Scar Massage
(Start Once the Incision Is Fully Healed)
Scar massage is often forgotten — but it plays a major role in recovery!
Scar Massage Helps:
Increase local blood flow
Improve scar mobility and flexibility
Reduce tightness or “pulling” sensations
Improve fluid movement and reduce swelling
Support nerve recovery
Potentially improve cosmetic appearance
When to Start Scar Massage
Only begin when:
The incision is fully closed
No scabs
No open areas
No stitches remaining
No signs of infection
Scars remodel for up to 2 years, so it’s never “too late” to improve mobility.
For new scars:
2–3 times per day for the first 3 months
Then reduce to several times per week
Stop if you notice:
Increased redness lasting >1 hour
Skin breakdown
Increased pain that persists
How To Do Scar Massage:
Preparation
Best after a warm shower
Use a dime-sized amount of unscented lotion, Vitamin E cream or the Vivier V-Stat Advanced Repair Gel
Finger Position
Use 2–3 flat pads of your fingers (index + middle, or index + middle + ring)
You should be able to see your fingernails.
If you can’t see them, you’re pressing too deeply.
Pressure
Moderate pressure.
The skin around your fingernail should turn slightly white.
Again — test on another body area first if sensation is reduced!
The 5-Minute Scar Massage Method
Set a timer and change direction every minute:
Minute 1:
Move fingers in small circles clockwise along the scar.
Minute 2:
Small circles counterclockwise.
Minute 3:
Slide fingers right to left along the scar line.
Minute 4:
Slide fingers left to right along the scar line.
Minute 5:
Move fingers perpendicular across the scar (cross-friction).
Tip: The scar should move under your fingers. If it doesn’t, stay consistent — mobility improves over time.
What If My Abdominal Scar Feels “Stuck” or Like a Shelf?
Once you can tolerate the 5 minute scar massage you can move into some more advanced techniques.
This is especially helpful if you feel:
Pulling with standing upright
Discomfort during core exercises
Tightness during twisting or reaching
Here are two more techniques to try:
Make it stand out
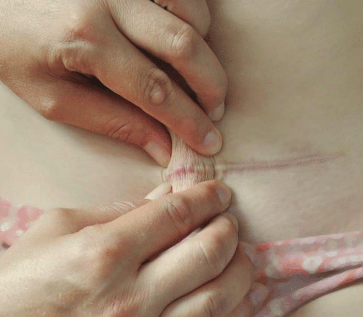
a. Skin Rolling:
Gently lift the skin above and below the scar.
Roll the tissue between your fingers.
Practice gentle skin lifting (if comfortable).
Work in multiple directions — not just along the scar line.
3. Scar Appearance
(Start Once the Incision Is Fully Healed)
The above techniques will help with the scars appearance but there are two other things you can use as well.
Once the dressings are off and there are no stitches, steri-strips scabs or infections you can apply either scar tape or scar gel.
The scar gel I recommend is the Vivier V-Stat Advanced Repair Scar Gel. It’s easy to apply, silicone based and I’ve seen great results from it (both personally and with my patients). I recommend applying a pea sized amount to your finger and gently massage it on daily until the scars appearance softens and fades.
Silicone scar tape is another option if you prefer not to use the gel. This can be found at almost any drugstore or online retailer. Look for a silicone scar tape and I prefer ones that I can cut to match the size I need instead of a pre-cut strip. Cut a piece large enough to cover the scar. Keep it on for several days or until it loses adhesiveness. Then reapply. If you want each piece to last longer take it off to shower. This can be helpful if the scar is uncomfortable with pressure or when you are wearing clothing. It feels like a nice protective layer once the dressing is off. Most people find that wearing this for 3 months greatly improves their scars appearance.
When Should I Call My Physio?
Scar work should feel productive — not worse over time. Reach out to your physiotherapist if you notice:
🚩 Increased Pain That Doesn’t Settle
Pain that continues to build over several days
Pain that lasts longer than 1 hour after scar massage
Sharp, burning, or electrical pain that’s worsening instead of improving
🚩 Signs of Infection
Redness spreading around the scar
Warmth and swelling that is increasing
Pus or unusual drainage
Fever
(If you suspect infection, contact your surgeon or primary care provider promptly.)
🚩 The Scar Feels “Stuck” or Deeply Tight
You feel pulling with movement that limits your mobility
Core or strength exercises feel restricted
You notice a visible “shelf” (common with abdominal scars)
The skin doesn’t glide when you try to move it
This may mean the deeper layers need more specific manual therapy or guided exercises.
🚩 Persistent Numbness or Hypersensitivity
Ongoing numbness that hasn’t improved over several months
Touch feels painful or intolerable
Clothing rubbing over the scar is still uncomfortable
We can guide you through more advanced desensitization strategies.
🚩 Bulging or Pressure Around the Scar
A visible or palpable bulge
Heaviness or pressure that increases with coughing or lifting
This is especially important after abdominal surgery and may require assessment for deeper tissue support.
Most scars improve beautifully with simple, consistent care. If something feels “off,” you’re not overreacting — early guidance often makes recovery easier and faster.